The music world lost a legend when D’Angelo—the velvet-voiced soul artist behind Voodoo and Black Messiah—was taken far too soon by pancreatic cancer. His passing was a painful reminder that this disease does not discriminate. It doesn’t care about your talent, your legacy, or how much the world still needs you.
For many of us, this wasn’t an abstract headline. It was personal. I lost my grandfather to pancreatic cancer. When he was diagnosed, we had only a matter of months together before he was gone. I had just left school and didn’t have a job at the time, so I stepped in as one of his primary caretakers. Watching him fight to hold on to normalcy—while his body was quietly losing the battle—was one of the hardest things I’ve ever experienced.
What made it so brutal was the speed. Pancreatic cancer doesn’t give you much time to process, to plan, or to hope. By the time most people receive a diagnosis, the disease has often already spread. That’s what makes awareness so critical. The more you know, the better equipped you are to catch it early—or support someone who needs you most.
This post is for the community. For those who lost someone, for those who are scared, and for those who simply want to be informed. Because if D’Angelo could be affected by this, we are all vulnerable. And knowledge is how we fight back.
What Is Pancreatic Cancer?
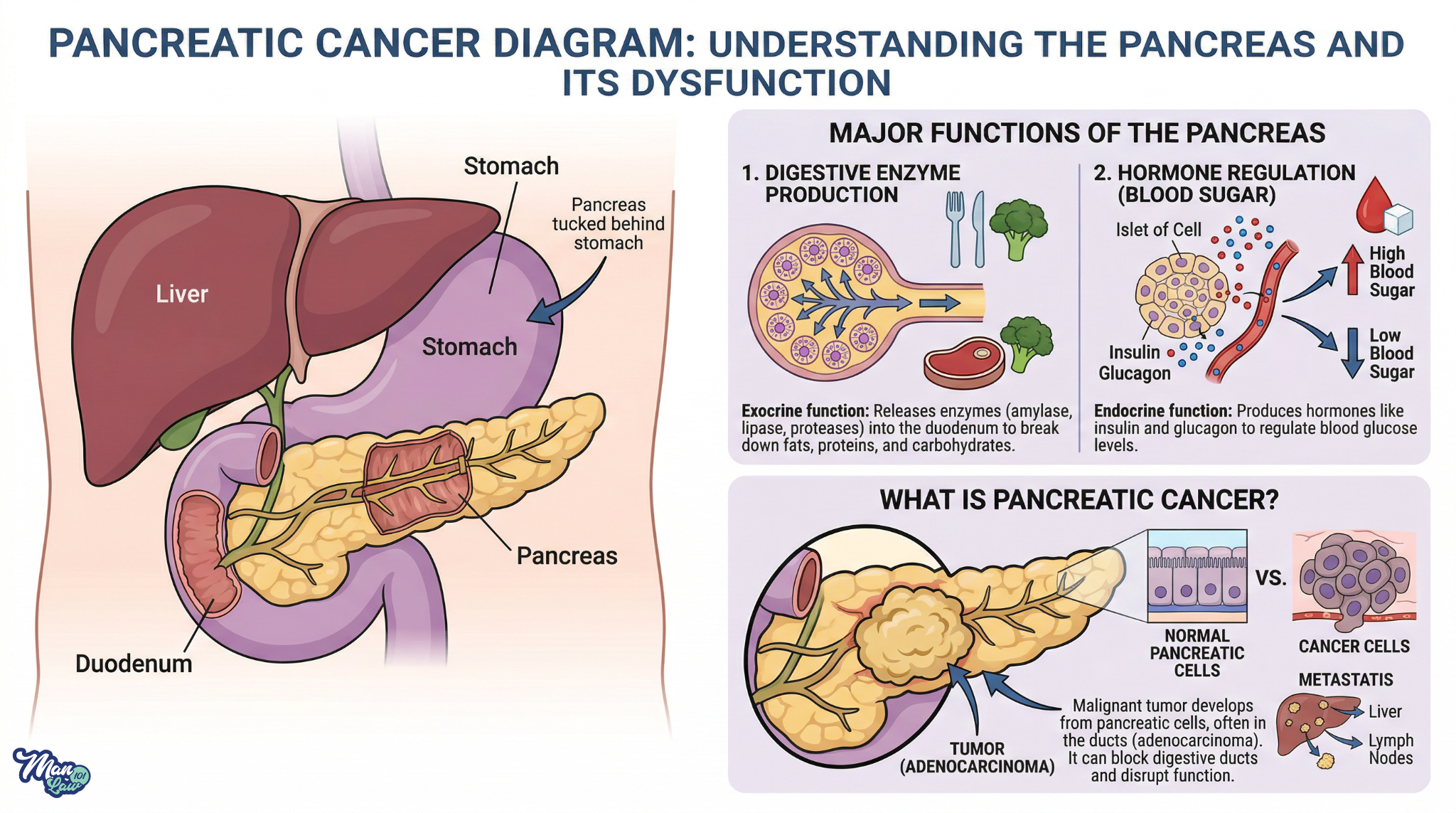
The pancreas is a glandular organ tucked behind the stomach. It serves two major functions: producing digestive enzymes that break down food, and releasing hormones like insulin that regulate blood sugar.
Pancreatic cancer occurs when abnormal cells in the pancreas grow uncontrollably and form a tumor. The most common type—accounting for roughly 90% of cases—is called pancreatic ductal adenocarcinoma (PDAC), which originates in the cells lining the pancreatic ducts. Other less common types include pancreatic neuroendocrine tumors (PNETs), which tend to grow more slowly.
What makes pancreatic cancer particularly dangerous is its location. The pancreas sits deep within the abdomen, making tumors difficult to detect through routine physical exams. There are also no reliable early-warning blood tests or widely recommended screening protocols for the general population. By the time symptoms appear, the cancer has often progressed to a later stage.
What Are the Symptoms of Pancreatic Cancer?
One of the most heartbreaking aspects of this disease is how silent it can be in its early stages. Symptoms often don’t appear until the cancer is already advanced—and even when they do, they’re easy to mistake for less serious conditions.
Common symptoms include:
- Jaundice (yellowing of the skin and eyes): Often one of the first noticeable signs, caused by a tumor blocking the bile duct
- Unexplained weight loss: Losing weight without trying, especially if combined with a loss of appetite
- Abdominal or back pain: A dull, persistent ache that can radiate from the abdomen to the back
- Digestive problems: Nausea, bloating, or changes in bowel habits, including oily or pale-colored stools
- New-onset diabetes: A sudden diagnosis of diabetes—especially in people over 50 with no other risk factors—can sometimes be an early warning sign
- Fatigue: Deep, persistent tiredness that doesn’t improve with rest
- Dark urine or light-colored stools: Both linked to bile duct obstruction
If you or someone you love is experiencing a combination of these symptoms—particularly jaundice alongside abdominal pain or unexplained weight loss—speak to a doctor as soon as possible. These symptoms don’t always mean cancer, but they deserve immediate attention.
Who Does Pancreatic Cancer Affect the Most?
Pancreatic cancer can affect anyone, but certain groups face a higher risk.
Age and Gender
The risk of pancreatic cancer increases significantly with age. Most diagnoses occur in people over 65, with the average age at diagnosis being around 70. Men are slightly more likely to develop the disease than women, though the gap has narrowed in recent years.
Does Pancreatic Cancer Affect Black Men More?
Yes—and this is a conversation the community needs to have openly. According to the American Cancer Society, Black Americans are diagnosed with pancreatic cancer at higher rates than any other racial or ethnic group in the United States. Black men, in particular, face a disproportionately elevated risk.
Researchers believe this disparity is linked to a combination of factors: higher rates of type 2 diabetes, smoking, and obesity within the community; limited access to quality healthcare and early screening; and potential genetic factors that are still being studied. Systemic barriers to healthcare access play a significant role, too—meaning that by the time many Black men receive a diagnosis, the cancer is already at an advanced stage.
This is why awareness and advocacy within Black communities are so important. D’Angelo’s passing is a call to action.
Other High-Risk Groups
Beyond race and age, other factors that increase risk include:
- A family history of pancreatic cancer or certain genetic syndromes (such as BRCA2 mutations)
- A personal history of chronic pancreatitis or type 2 diabetes
- Smoking (smokers are roughly twice as likely to develop the disease)
- Obesity and a sedentary lifestyle
- Heavy, long-term alcohol use
What Causes Pancreatic Cancer?
There is no single definitive cause of pancreatic cancer. Like most cancers, it develops when DNA mutations cause cells to grow abnormally. Some of these mutations are inherited; others are acquired over a lifetime through lifestyle and environmental exposure.
The main risk factors currently identified include:
- Smoking: One of the most significant modifiable risk factors
- Obesity: Excess body weight, especially around the abdomen, is linked to increased risk
- Type 2 diabetes: Both a risk factor and, in some cases, an early symptom
- Chronic pancreatitis: Long-term inflammation of the pancreas
- Genetic mutations: Inherited mutations in genes like BRCA1, BRCA2, PALB2, and ATM have been linked to a higher risk
- Family history: Having a first-degree relative with pancreatic cancer increases your risk
It’s important to note that many people diagnosed with pancreatic cancer have no obvious risk factors. That’s what makes this disease so unpredictable—and why general awareness matters for everyone.
Is There a Cure for Pancreatic Cancer?
This is the hardest part of the conversation. Currently, there is no guaranteed cure for pancreatic cancer. However, treatment options do exist, and survival rates are improving—slowly but meaningfully—as research advances.
Treatment options include:
- Surgery: The Whipple procedure (pancreaticoduodenectomy) is the most common surgical approach and offers the best chance of long-term survival, but it is only possible when the cancer is caught early and has not spread.
- Chemotherapy: Often used before surgery to shrink tumors, or after surgery to reduce recurrence risk. FOLFIRINOX and gemcitabine-based regimens are commonly used.
- Radiation therapy: Sometimes used in combination with chemotherapy.
- Targeted therapy: Drugs that specifically target genetic mutations, such as PARP inhibitors for those with BRCA mutations.
- Immunotherapy: Still largely in the experimental phase for pancreatic cancer, but showing promise in clinical trials.
The five-year survival rate for pancreatic cancer currently sits around 12–13% overall, but this number climbs significantly when the disease is caught at a localized stage—before it has spread. That number is proof that early detection saves lives.
Clinical trials are expanding, and organizations like the Pancreatic Cancer Action Network (PanCAN) are funding research and connecting patients with cutting-edge treatment options. If you or someone you love has been diagnosed, exploring a clinical trial may be worth discussing with an oncologist.
How Often Should I Get Screened for Pancreatic Cancer?
Here’s the difficult truth: there is currently no recommended routine screening for pancreatic cancer in the general population. Unlike breast or colon cancer, no standard test has proven effective enough for widespread use.
However, high-risk individuals should be screened. If any of the following apply to you, speak to your doctor about a personalized surveillance plan:
- A family history of pancreatic cancer (especially two or more affected relatives)
- A known genetic mutation linked to pancreatic cancer (BRCA1/2, PALB2, ATM, Lynch syndrome, etc.)
- A personal history of chronic pancreatitis or hereditary pancreatitis
For high-risk individuals, screening typically involves an annual endoscopic ultrasound (EUS) or MRI, starting at age 50—or 10 years younger than the youngest affected family member.
For everyone else, the best defense is managing modifiable risk factors: quit smoking, maintain a healthy weight, limit alcohol, and manage diabetes if you have it. Most importantly, pay attention to your body. If something feels off, don’t wait.
Frequently Asked Questions
Is pancreatic cancer always fatal?
Not always, but it is one of the most serious cancer diagnoses. When caught early, before the cancer has spread, surgery can be curative for some patients. The challenge is that early-stage pancreatic cancer rarely causes noticeable symptoms, so most cases are diagnosed at a later stage.
Can young people get pancreatic cancer?
Yes, though it is far more common in older adults. Cases in people under 40 are rare but do occur, particularly in those with inherited genetic mutations or a strong family history.
What should I do if a family member has pancreatic cancer?
First, be present. Caregiving for someone with pancreatic cancer is demanding, both physically and emotionally—just as I experienced with my grandfather. Connect with support resources like PanCAN’s Patient Services (1-877-272-6226) for guidance on treatment options, financial assistance, and emotional support. And speak to your own doctor about your personal risk level given your family history.
Are there support communities for people affected by pancreatic cancer?
Yes. Organizations like PanCAN, the Hirshberg Foundation, and Let’s Win PC offer patient communities, caregiver resources, and advocacy networks. You don’t have to navigate this alone.
Knowledge Is How We Honor the Ones We’ve Lost
Losing D’Angelo to pancreatic cancer was a gut punch to the culture. Losing my grandfather was a wound that changed me. But grief, when channeled with intention, can become something powerful.
Talk to your doctor about your risk. Know the symptoms. Advocate for yourself in medical spaces where Black voices have historically been dismissed. Share this post with someone who needs it. Check on the people you love.
Pancreatic cancer moves fast—but so can we. Let’s get ahead of it.
Resources:
- Pancreatic Cancer Action Network (PanCAN): pancan.org
- American Cancer Society: cancer.org
- National Cancer Institute: cancer.gov




